ME/CFS is a multi-system disease
ME/CFS Symptoms
Not only do symptoms vary in type but also in severity, ranging from mild to severe. An estimated one in four patients are housebound or bed bound and many of the most severely affected need to be fed by tube.
There are over 60 symptoms reported by people with ME/CFS. The common symptoms are listed but not limited to what may define an individual experience.
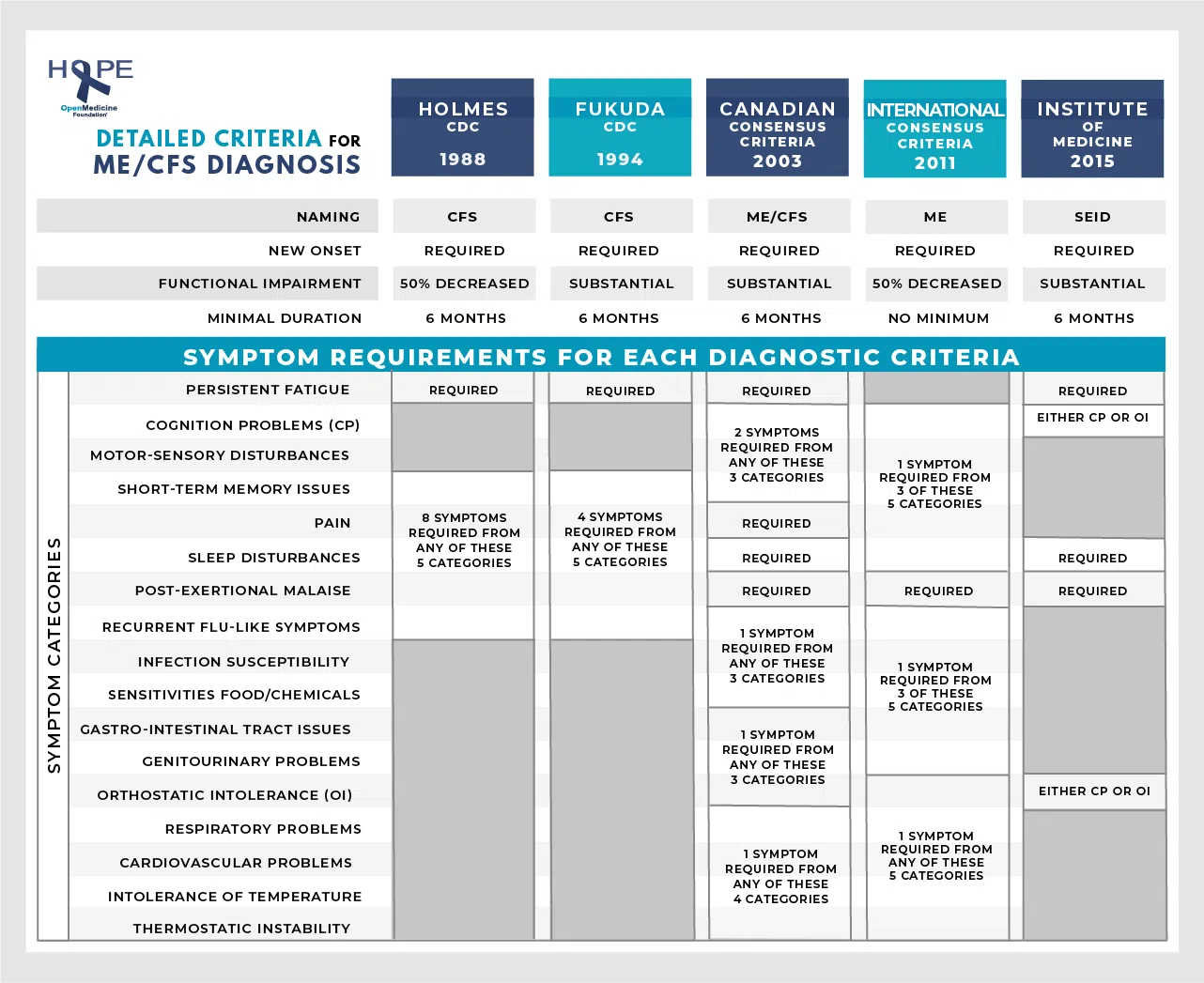
Currently, there is no laboratory diagnostic test. Due to a symptom set that overlaps with several other diseases, clinical assessment and symptoms and the exclusion of other diseases are necessary for accurate diagnosis.
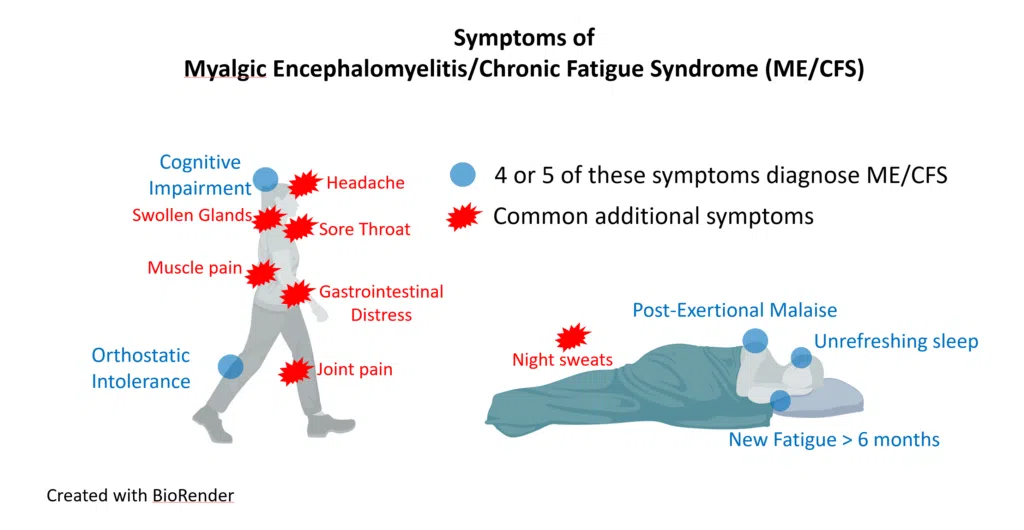
Most Common Symptoms
Main Diagnostic Symptoms
Post-exertional malaise (PEM) - symptoms worsen after exertion
Reduction or impairment in ability to carry out normal daily activities, accompanied by Profound Fatigue
Unrefreshing sleep
Cognitive Impairment
Orthostatic intolerance (symptoms worsen when sitting or standing upright)
Severe body pain and worsening headaches